Living with myasthenia gravis (MG) may be preventing you from doing the things you love. This article and downloadable discussion guide can help you work with your doctor to find a management plan that could suit your personal goals
It may be difficult to explain to your healthcare team how your MG symptoms are affecting your lifestyle, but it’s an important step in finding the best management plan for you. Discussing your symptoms, goals and how MG impacts your daily activities may help your healthcare team understand what’s going on in your life and if they should consider making changes to your myasthenia gravis management plan. Consider the tips in this article and the downloadable discussion guide to help organize your thoughts and guide a successful conversation with your doctor. You are your own best advocate, and when your doctor understands you, it may be easier for them to prioritize the things that matter most to you.
Step 1: Write down your symptoms
You may find it helpful to take a few minutes to prepare for your next appointment by writing down your symptoms to help you get the most out of your visit. Have your symptoms limited your ability to complete your favorite hobby or reduced social interactions? Having your symptoms written down may help start the conversation with your doctor.
Step 2: Think about what matters most to you
Think about how your symptoms interfere with your ability to complete day-to-day tasks and activities and how this impacts your ability to work toward your goals. Do you have plans that you want to make with regards to working or seeing your friends and family? Share what you’ve been looking forward to doing and try being as specific as possible. The extra details may help your doctor understand what’s going on and if they should consider changing plans.
For example, instead of saying “I’m frequently tired,” you might try, “I’m unable to walk my dog because of my muscle fatigue and would like to get back into that routine.” Or, “My muscle weakness prevents me from walking and going to the grocery store to buy butter and I’d love to start baking again.” Using more specifics like, “My double vision prevents me from driving, and I want the independence to see my family again” may give your doctor a better picture of what you’re experiencing.
Your doctor wants to hear how you’re doing and what your priorities are. Including examples may change the picture in terms of what your doctor sees. Dr. Erika P. Greene said that “patients fall into a new normal after diagnosis and that doctors take that new normal and remain content over time,” however, she encourages you to, “open back up the conversation… and ask yourself if you are satisfied with your symptoms or abilities and if there is room for improvement.”
Readdressing your expectations and needs is important in being your own advocate and ensuring that you are in the driver’s seat when it comes to your goals. Having an open dialogue with your doctor about symptoms and how they affect your day-to-day living is at the heart of patient-centered care. It takes teamwork to create your unique management plan.
Thinking about your expectations and adding in these specifics may help your doctor better tailor your management plan toward meeting your personal goals. Remember that the better they understand what you’re going through, the better they’ll be able to support you.
Step 3: Prepare for your next discussion with your doctor
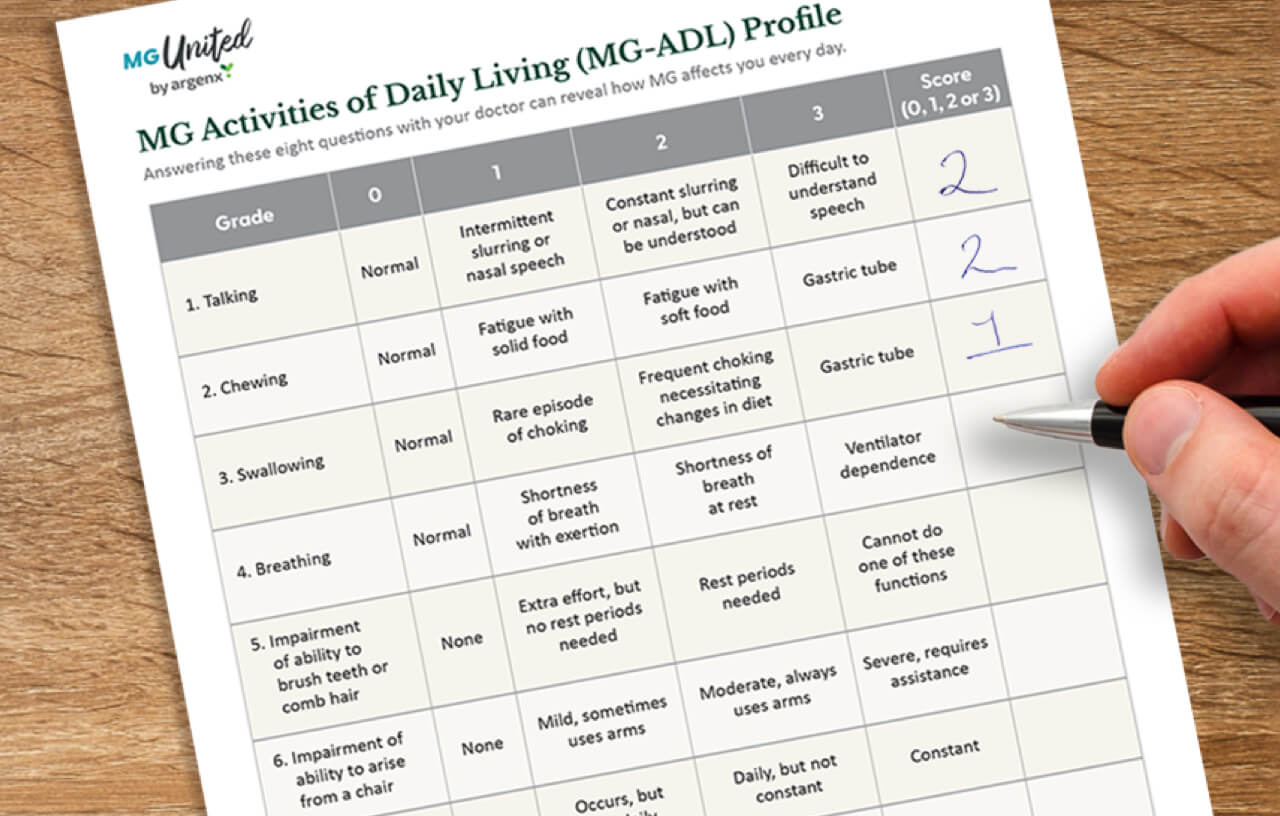
Download and fill out the doctor discussion guide below or take pictures of it on your phone and bring it to your next appointment to help you have a productive conversation with your doctor.
You can also take the healthcare communications quiz to find out how effective your communication style is and discover more tips on partnering with your doctor.